Explore essential strategies for managing atopic dermatitis with our expert guide. Learn about symptom relief, trigger avoidance, and maintaining healthy skin.
Normal, dry to atopic skin
Atopic Dermatitis : Symptoms, Factors & Treatments
Reading time : 8 min
Atopic Dermatitis : A Complete Overview
Atopic dermatitis, often referred to as eczema, is a condition that causes dry, itchy and inflamed skin. Discover how to manage atopic dermatitis and find solutions to limit the symptoms.
Understanding Atopic Dermatitis
Atopic dermatitis is a chronic disease that causes inflammation, redness and irritation of the skin. It is common for young children between 2 months and 5 years old, but it can start at any age. Atopic dermatitis is not contagious and can overlap with other types of eczema.
Atopic Dermatitis vs. Eczema:
Atopic dermatitis is often called eczema, but it is one of the different types of eczema. Eczema is in fact, a general term for rash-like skin conditions.
Indeed, there are several types of eczema and atopic dermatitis is the most common type. Other types of eczema include contact dermatitis and stasis dermatitis.
Both eczema and atopic dermatitis start out as dry and itchy skin, but they may become worse. Rashes can appear anywhere on the body and ooze, weep fluid and bleed when scratched, making skin vulnerable to infection.
You will surely be interested in
Symptoms and Manifestations
The symptoms of atopic dermatitis include dry skin, itchiness, rashes, bumps and crusting. These symptoms can appear anywhere on the body. Skin can become dry and discolored, and repeated scratching can cause thickening. Because of its chronic nature, atopic dermatitis can be a real burden on everyday life.
The most common symptoms of atopic dermatitis are:
Dry and cracked skin
Itchy skin
Rashes on swollen skin
Atopic dermatitis is often very itchy and there are times when the condition gets worse because of scratching. Your skin can turn red and inflamed. A clear fluid may even leak from the rash. Eventually, the rash will crust over and start to scale.
Complications of atopic dermatitis can happen and lead to:
Bacteria skin infections or viral skin infections
Irritant hand dermatitis
Allergic contact dermatitis
Sleep loss because of scratching
Conjunctivitis or blepharitis
Asthma and hay fever
Food allergies
Mental health conditions
Variability Across Dermatitis Types:
The symptoms can vary depending on the type of dermatitis and the severity. There are many dermatitis types, and they all have their own symptoms, triggers and treatments
Contact dermatitis is an itchy rash caused by direct contact with a substance or an allergic reaction to it. Contact dermatitis shows up on skin that has been exposed to the substance. Symptoms can include itchy rash, leathery patches, dry and cracked skin, bumps and blisters, swelling and burning
Dyshidrotic eczema is a skin condition that causes small blisters on the palms of hands, soles of the feet and edges of the fingers and toes.
Nummular eczema is characterized by scattered circular, itchy and oozing patches. The spots can look coin-shaped on the skin.
Seborrheic dermatitis is a common form of eczema that usually affects the scalp with dandruff. It can turn into a rash on the affected areas.
Neurodermatitis is usually confined to one or two extremely itchy patches of skin, and it rarely goes away without treatment. It is a condition that causes patients to scratch even when they don’t realize it. Scraping lights up their brain’s reward center and it becomes in some sense, pleasurable.
Stasis dermatitis happens when there is a venous insufficiency or poor circulation in the lower legs. It can be caused by aging, but it can also signal a serious underlying medical condition such as heart or kidney disease.
Provoking Factors
Atopic dermatitis can be caused by different factors like genes variation, bacteria Staphylococcus, or weak skin barrier function.
Risk Factors
When you already have eczema, allergies, hay fever or asthma, you are more inclined to develop atopic dermatitis.
Heredity also increases the chance of atopic dermatitis. Indeed, if there is a family history of atopic dermatitis, the chance of developing this condition is higher.
Finally, research shows that atopic dermatitis is more common in white European children and that girls tend to develop the condition slightly more often than boys.
Eczema in Infants
Atopic dermatitis often appears between 2 months and 5 years of age. It is most common for children to develop a red rash on the face, scalp and areas of skin around joints.
Babies with a light skin tone often develop atopic dermatitis on their face. Pink or red rashes with bumps and swollen skin usually appear around their mouth.
Babies with darker skin tone are more likely to develop small bumps with dry skin.
During childhood, the red thickened rash develops on the elbows, knees, neck and ankles and may ooze or bleed when scratched.
Atopic dermatitis in infants and children can be triggered by eating certain foods such as eggs or cow’s milk
Duration of Atopic Dermatitis
Atopic dermatitis is a chronic disease which can last for a long time. The disease normally goes away by the teenage years but for some people, it lasts for life. It is impossible to determine if dermatitis will become a lifelong condition, but you can prevent the symptoms from getting worse.
Genetics and Environmental Influences:
Environmental factors may trigger the immune system to change the protective barrier of the skin. These factors can include:
Smoke
Air pollutants
Fragrances and other compounds found in skin product and soaps
Genetics also play a role in atopic dermatitis, and researchers found that changes to genes can impact skin barrier. These changes expose the skin immune system to environmental factors leading to atopic dermatitis.
Always at your side to guide you
Recognizing Triggers and affected areas
Atopic dermatitis can develop on different parts of the body like the face, joints, skin folds, chest, hands and feet.
Each person diagnosed with eczema has unique triggers that cause the symptoms to flare up.
The most common triggers for atopic dermatitis are:
Dry skin and skin infection
Heat and sweat
Stress
Irritants like fabrics, cleaning products, fragrances...
Dust mites, pet dander, mold
Cold and dry air
Pollen
Smoke
Atopic dermatitis can cause a very itchy rash behind the knees. Joint areas are particularly affected by eczema because of skin rubbing against each other. This irritation behind knees can result from crawling for babies or walking for adults.
Other triggers include extended exposure to extreme temperature resulting in sweat, certain types of soaps, certain chemicals such as laundry detergents, certain fabrics such as wool and polyester, dust mites.
Moisturizing creams and topical corticosteroids can help relieve symptoms.
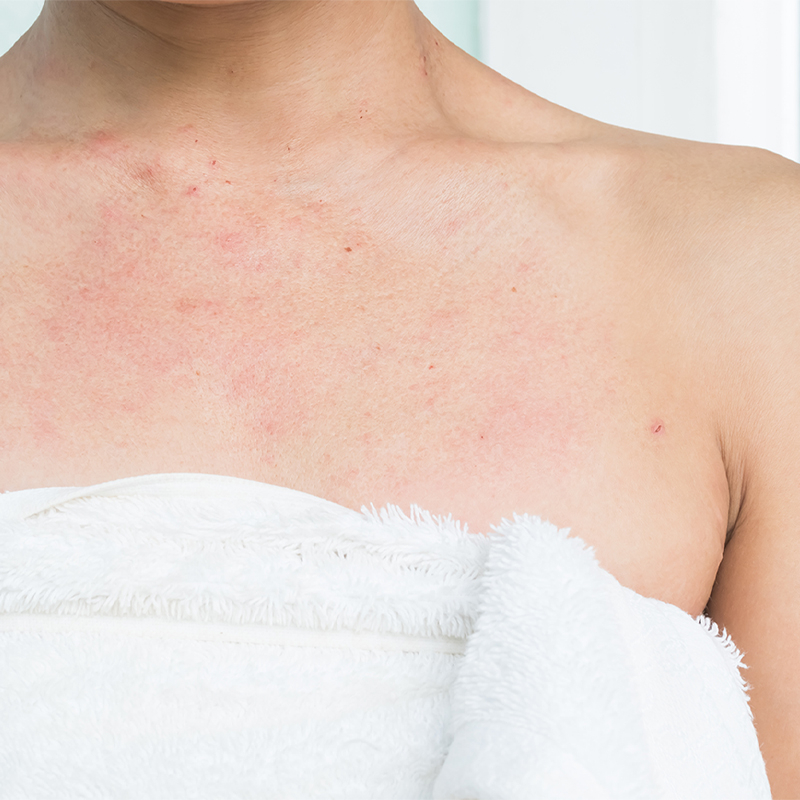
Dermatitis can appear on the chest which is a part of the body that contains a lot of sebum. Rash, dryness, itching and redness are the main symptoms of dermatitis on the chest.
Some factors as yeast infection, sebum production, dry weather, stress, hormonal changes and medical conditions appear to play a role in dermatitis.
Hand and foot dermatitis is a chronic disease characterized by red, scaly, thickened skin on the hands and/or feet.
The symptoms are redness, scaling and thickening of the skin on the hands and feet. They often progress as blisters called dyshidrotic dermatitis.
The treatment can include corticosteroids, phototherapy and antibiotics. If the cause is known, avoiding contact with the allergen will help avoid the symptoms
Intertriginous dermatitis, also called intertrigo, is an inflammatory condition of skin folds aggravated by heat, moisture, maceration, friction and lack of air circulation. The skin-to-skin friction causes inflammation, rashes and itchiness.
The treatments include skin barrier cream, topical steroid cream and antibiotics in case of infection.
Treatment Options: How to soothe the skin?
Atopic dermatitis cannot be cured but medications and daily management can ease the symptoms.
Medications and Creams
Developing a basic skin care routine with ultra nourishing creams may help prevent atopic dermatitis flares.
Keep your skin moisturized with a daily skincare, like creams, shea butter or any other products which are gentle and compatible with your symptoms. BIODERMA Atoderm Ultra cream is, for example, one of the daily skincare you can use to strengthen your skin barrier.
Apply an anti-itch cream to help you avoid scratching and relieve the inflammation.
If these are not enough, other medical treatments can include:
Topical corticosteroids
Non-steroidal topicals
Finally, in serious cases of atopic dermatitis, your health care provider may prescribe antibiotics or injectable biologics to treat the infection and control inflammation.
Complementary Therapies
Different therapies can also be considered as an alternative to medication for atopic dermatitis symptoms.
Wet dressing is an effective treatment which involves corticosteroid ointment. It is done in a hospital for people with widespread lesions.
Light therapy is used for people who cannot use medical or topical treatments. This phototherapy involves exposing the affected areas to natural sunlight to limit the symptoms.
Counseling can be a good option if you feel embarrassed or frustrated by your skin condition.
Daily Management
Adopting a new lifestyle and home remedies help reduce itching and soothe inflamed skin. When atopic dermatitis is not too severe, daily management steps can be followed such as:
Avoid known triggers
Reach high quality sleep
Follow a healthy diet
Manage stress
Favor daily bath or shower with warm water rather than hot water
Use gentle and non-soap cleanser twice a day
Don’t scratch
Avoid any irritating products
Use a humidifier
Wear cool, smooth-textured clothing
Treat stress and anxiety
As we saw throughout this article, atopic dermatitis is often a vicious cycle of itching and scratching leading to inflammation and further damage to the skin barrier. It can have a huge impact on quality of life making it difficult to concentrate or sleep. No cure has yet been found but hopefully there are many treatments and precautions that can help you relive your symptoms and improve your everyday life.